High-Tech Help for Facial Pain
When traditional medicine and surgery can't do the job, doctors turn to cyberknife.
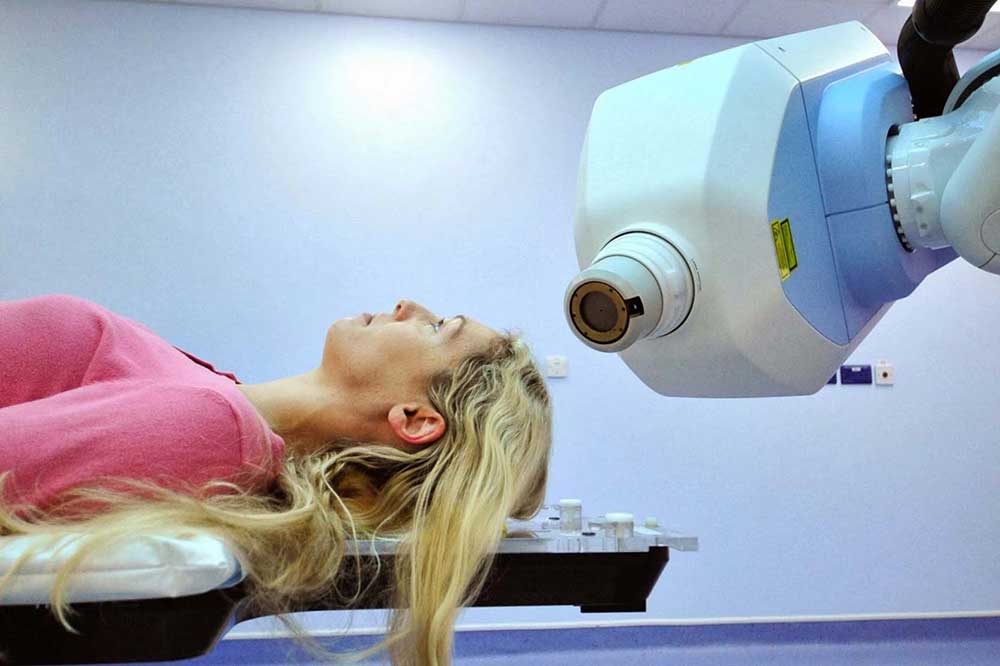
A light breeze on the cheek. A sip of a drink. Smiling at a friend. Simple as they are, these everyday occurrences involving slight facial movement can trigger a severe, debilitating jolt of pain for some people. They have a condition in which a key nerve in the face, the trigeminal nerve, is damaged.
“The pain can be excruciating,” says Alison Grann, M.D., chairman of Radiation Oncology at Saint Barnabas Medical Center. “It may occur a couple of times a day at first. But over time, those jolts of pain can happen much more often.”
People with the condition, called trigeminal neuralgia, describe the pain as a burning, an electric shock or a jolt of lance-like pain. Traditional pain medicines do not usually work. Other types of medicines and surgery can be effective for most, Dr. Grann says.
“However, a small number of people try every conventional option they can find and still don’t get relief,” she says. For these patients there is now an advanced treatment available at Saint Barnabas Medical Center. “We use CyberKnife stereotactic radiosurgery to target the nerve without the need for traditional surgery,” explains Dr. Grann. “And for patients who are not healthy enough for surgery, this may be the only option.”
The CyberKnife system employs a continual image guidance software that allows it to deliver high radiation doses with pinpoint accuracy, while automatically correcting for tumor movement. Because radiation beams are adjusted in real time to the patient’s breathing cycle, damage to surrounding healthy tissue is minimized.
Trigeminal neuralgia affects about five out of 100,000 people a year. Damage to the nerve can result from a blood vessel or tumor pressing on it; a disease such as multiple sclerosis or an injury, surgery or stroke may also be the cause.
The condition most often comes on suddenly and causes shooting pain. It may also cause a more constant dull, aching or burning sensation. Women are more likely to develop it, as are people over age 50.
The trigeminal nerve runs across almost the entire face and is near other important nerves, blood vessels, muscles and structures. So accuracy in treatment is extremely important, Dr. Grann says.
“The planning for radiosurgery is complex,” she says. “For each patient, we meet daily before the day of treatment to review the plan and to make any adjustments.” (See “Super Tool, Super Team,” above.)
With either traditional surgery or radiosurgery, pain relief can be excellent. Pain can recur over time. But for many, relief is long-term.
“For our patients who cannot have surgery or do not want it, radiosurgery does provide a good option,” says the doctor. “CyberKnife treatment is a valuable addition to our technology to help patients regain a higher quality of life.”
Super Tool, Super Team
CyberKnife stereotactic radiosurgery is a technology physicians use to aim high doses of radiation at particular cells or tissues, often malignant ones. (“Stereotactic” refers to locating a very small point inside the body using many different angles, while “radio” in this instance refers to radiation.) It is most commonly used to treat patients with cancer, but specialists at Saint Barnabas Medical Center have put a team in place to take advantage of the system’s advancements to treat other conditions too. (See main article.)
“Treatments using stereotactic radiosurgery are incredibly complicated,” says Alison Grann, M.D., chairman of Radiation Oncology at Saint Barnabas Medical Center. “It uses extremely high doses of radiation aimed at an area of tissue that is very small. But the tissue is surrounded by important nerves, muscles and tissues. That complexity is why patients need a facility like Saint Barnabas Medical Center with staff that specializes in radiosurgery.”
During the outpatient procedure, physicians use sophisticated software that works with sensors in a patient’s customized facemask, which is made of see-through mesh. Other radiosurgery systems used elsewhere rely on a helmetlike “frame” that is actually screwed to the head. With the CyberKnife, the team combines information from the mesh mask and medical images taken in real time in the operating room to determine the exact size, shape and location of the treatment area.
Using this information, the CyberKnife’s GPS-like computer navigation (like that used in a car or an electronic map) helps doctors focus the beam where they need it. The system also tracks any movement of the patient—from breathing, for example—to avoid healthy tissue.
“We have a unique team here with extensive training in all aspects of care, and we have more than one set of eyes on every step of treatment,” Dr. Grann says.
The radiosurgery team at Saint Barnabas works under the close oversight of the radiation oncologist. Members include three Ph.D. physicists and three dosimetrists, who specialize in calibrating the delicate machinery, determining the best dose of radiation and planning the path that the CyberKnife will take to deliver it. Also important is the contribution of experienced radiation therapists and nurses.
In the days before a treatment, the entire team tests the plan, makes any adjustments based on the radiation oncologist’s review, and re-tests.
“In total, it might take us approximately a week to perfect each patient’s plan,” says Dr. Grann.
Physicians at the medical center have also been using CyberKnife for almost two years for patients with cancers of the prostate, lung, brain and pancreas.
For more information on use of cyberknife to treat facial pain, please call 973.322.5630 or visit rwjbh.org/sbmccyberknife.

 Alison Grann, M.D.
Alison Grann, M.D.